If you live or work in Denver, you've more than likely encountered Dr. Bill Burman's work.
Burman spent the last 10-plus years leading the public health arm of Denver Health, the city's safety-net hospital, and among his duties was making recommendations on public health orders in the city, like the one currently requiring you to wear a mask indoors.
Burman stepped down from his role this month.
On his last day on the job, Burman sat down with us to talk about the ongoing pandemic, the impact of the new variant, and the work he will continue to do on a part-time basis for the hospital, where he's worked since 1995.
His outgoing message about the pandemic is a sobering one, especially in light of comments Gov. Jared Polis made to CPR News earlier this month about the pandemic being over as an emergency,
"We are not done with this, period," Burman said. "There is no doubt we are not done with this. And so maybe the governor meant something different, but we were and are concerned about any messaging which says in some way, 'We're through this.' We're not."
He noted that the omicron variant is more contagious than previous variants.
"One thing I think we can be absolutely certain about is it is more transmissible, and not a little bit, a lot," Burman said about omicron, which was detected in Denver earlier this month, prior to this interview.
Omicron is raising concerns about potential spikes in hospitalizations, and one way Denver Health is preparing is making sure hospital beds are used appropriately.
"One of the major challenges this hospital faces, and I'm sure it's true for other hospitals, is difficulty transferring patients out who no longer need an acute hospital bed level of care," he said.

Another area of focus for the hospital will be monitoring the mental health of its staffers. A potential new wave is discouraging, Burman said. One way the hospital is trying to make sure they pay attention to its staff's wellbeing is through a program called Resilience in Stressful Events, or RISE, which provides free and confidential counseling sessions.
As for the general public's response to the new variant, Burman suggests going back to the basics: Make sure you're vaccinated, and if you are already vaccinated, get a booster. He said to think carefully about your holiday plans to try and reduce the risk of transmission. Consider smaller groups and meeting outside.
In some ways, Burman's research into HIV has helped him navigate the pandemic.
When Burman was offered the job as public health director in 2011, he wasn't interested. He said he was comfortable in the clinical field. But he agreed to take on the role and quickly realized he'd enjoy it.
"It was exciting to be in totally new areas to be doing things, having to learn things that I didn't know anything about: childhood obesity, paternal child health, tobacco, substance use disorders, mental health," Burman said. "It was, and is, initially uncomfortable, but then a great challenge to try to learn both the subject and the people."

When the HIV pandemic started, Burman remembers hearing from patients who faced what he called inhumane treatment, including hospital staff members who would try and spend as little time as possible inside a room with an HIV-positive patient. He lauded the role activists played during this era, drawing attention to the condition and ensuring good treatment for people who were HIV positive.
"It was a tremendous lesson of the need to work so much more closely with the community to have the true ground sense of what's happening, what's needed, what kind of research is needed," Burman said. "It's an absolute requirement. You cannot respond to a pandemic like COVID if you haven't built bridges to parts of your community."
Dr. Sarah Rowan, associate director of HIV and viral hepatitis prevention at Denver Health, said Burman learned Spanish later in life and took regular lessons with a tutor to serve Spanish-speaking patients. He worked at the Tepeyac Community Health Center, overseeing their HIV program. Rowan saw him work at the clinic firsthand and said he served as a mentor for people at the hospital. He'll continue to conduct HIV research for the hospital on a part-time basis.
"I think he really stepped outside his life perspective for his patients," Rowan said. "He set a good example of doing that."
Burman also served as chief medical officer for the city, consulting regularly with the Denver Department of Public Health & Environment Executive Director Bob McDonald about the public health orders issued by the city during the pandemic.
"He's one of the sharpest public health professionals I've ever met," McDonald said in a statement to Denverite. "What a huge asset he was to DDPHE, the region, and the state. He's very well known and respected, and he will be missed."
Burman said the pandemic hasn't shown new problems in our society, bur rather shone a light on them.
To start: access to universal healthcare. Burman used free COVID-19 testing, which the city started offering last year, as an example.
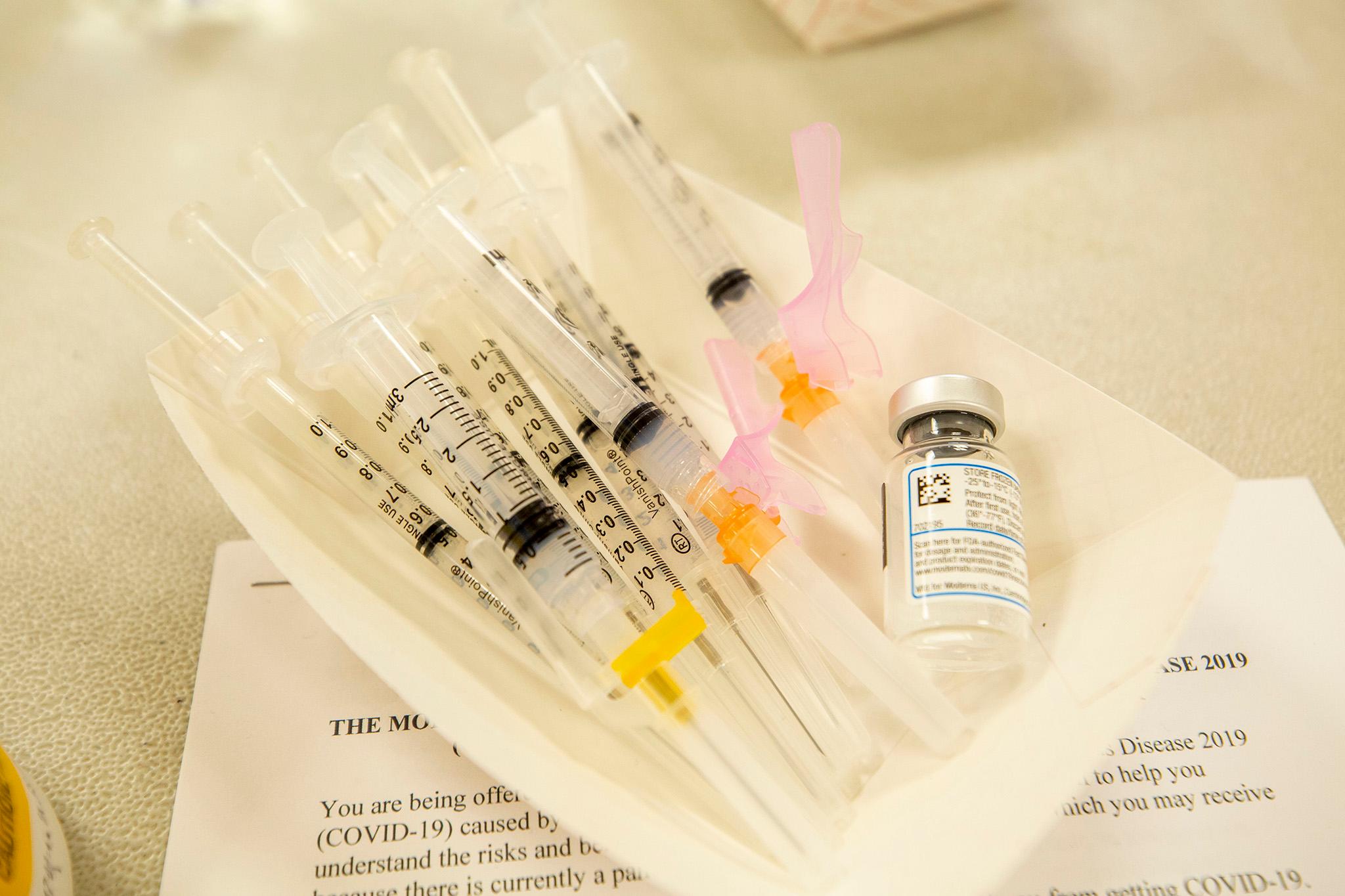
"Well, if you don't have health insurance, you have an understandable reluctance to be tested," Burman said. "Even if somebody says it's free, is that really free? Why would we give away anything in America for healthcare? We don't generally. You're also concerned about, is this gonna then engender downstream costs if I test and I test positive? And so I think that's been a problem forever. And to me, COVID just shone the spotlight on the gaps in our care system, when we don't have universal access to healthcare. It is way past time for us to do that."
Burman was responsible for improving regional work between other metro area public health agencies, helping launch the Metro Denver Partnership for Health in 2013. The group has advocated for measures to combat the pandemic, including asking the governor to implement a statewide mask mandate and require vaccine passports for most indoor settings.
That group used to meet once a month; it meets twice a week now. He said he's hopeful the group will continue to do good work.
"I leave with a sense of satisfaction," Burman said. "There are always uncertainties, but (I leave) with a real sense of satisfaction."