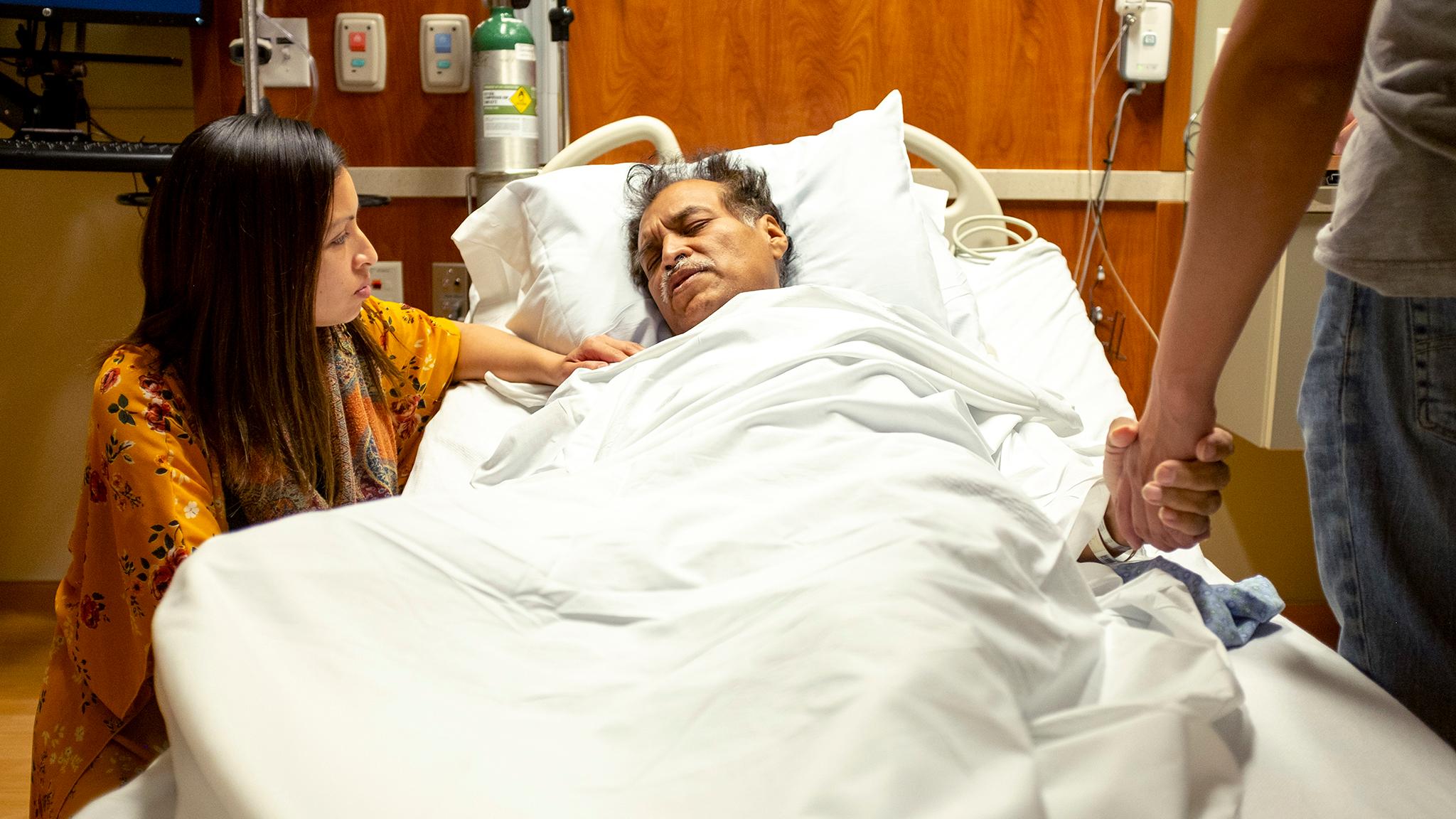
The future was uncertain for Armando Peniche-Cruz as he lay in an emergency room at St. Joseph Hospital last spring.
His children sat with him as doctors and nurses checked in. One spoke to him in Spanish about the pain that brought him in as he cleaned the bag, attached to Peniche-Cruz's stomach, where the contents of his gut were being diverted from his colon. He'd been in and out of ERs and clinics for the last year, but it wasn't until a few weeks before he landed at St. Joe's in City Park West that doctors finally diagnosed stage IV colorectal cancer. Weak and suffering, he was hoping he'd begin treatment.
"I can't go to work. I can't do nothing," he rasped. "This situation changed my life."
Peniche-Cruz is undocumented and uninsured. Preventative checkups were never in his cards. So, like many people in his situation, the emergency room was the only place he had access to care.
America's Dreamers, undocumented residents who came to the U.S. as children, have been allowed to remain and work in the country since President Obama created the Deferred Action for Childhood Arrivals program, known as DACA, in 2012. The fate of that program has been on the rocks since President Trump took office, and its constitutionality will be challenged before the U.S. Supreme Court within the next year. At the moment, DACA recipients can still work and use medical insurance that comes with those jobs.

But the parents of those Dreamers - people like Peniche-Cruz - have never had a pathway to legal employment and its benefits. As they age, they'll likely face difficulty accessing treatment when their health falters. For some, the answer may be to leave the country. Others may continue to visit emergency rooms where uninsured patients can get short-term care, sometimes on the taxpayer's dime.
People who can't afford insurance, including undocumented people, do have access to Emergency Medicaid. It offers minimal coverage that varies by state, but it can usually only be invoked for life-threatening conditions. Many people can't access it until diseases like cancer have progressed to later stages.
The Colorado legislature is exploring a state-run insurance option that aims to serve people who can't afford private coverage. As they've solicited input from people and businesses across the state, some groups have advocated that undocumented residents be allowed access to the program.
For now, an entire generation of underinsured, aging and undocumented residents are heading toward an increasingly uncertain fate.
Peniche-Cruz has put his body on the line for his three children their entire lives.
It began when they lived in Puebla, Mexico. They were poor -- poor enough that he and his wife gave up two meals each day to ensure their kids had enough to eat. After his wife left the family, he asked his children, Laura and Armando Jr., who were 13 and 9 at the time, if they'd support a move to the United States.
As young as they were, Laura said their father always consulted his children. They wanted to go. She wanted to be a filmmaker, and she knew that America meant Hollywood. Armando Jr. wanted a Nintendo 64. He said it was his "American Dream," and he carried a cut-out photo of the game system in his pocket all the way to Denver.
Peniche-Cruz carried his youngest son across the Rio Grande near Juarez as Laura and Armando Jr. waded beside them. They hid under a bush on the other side as a helicopter hovered above them, close enough that Armando Jr. remembers seeing the pilot's face. They lay beneath a car for hours until they felt safe enough to emerge. Then, Peniche-Cruz led them through the desert to evade a checkpoint, sometimes carrying both his sons at once, until they finally made it to the rendezvous spot where they caught a ride to Colorado.
"I remember looking at his feet, and they're just bleeding from being cut and from thorns and he's holding my two brothers," Laura recalled. "I tattooed that image in my memory, of this family who is walking in the dark, only lit by the light of the stars, and just being so faithful that this sacrifice is worth it."
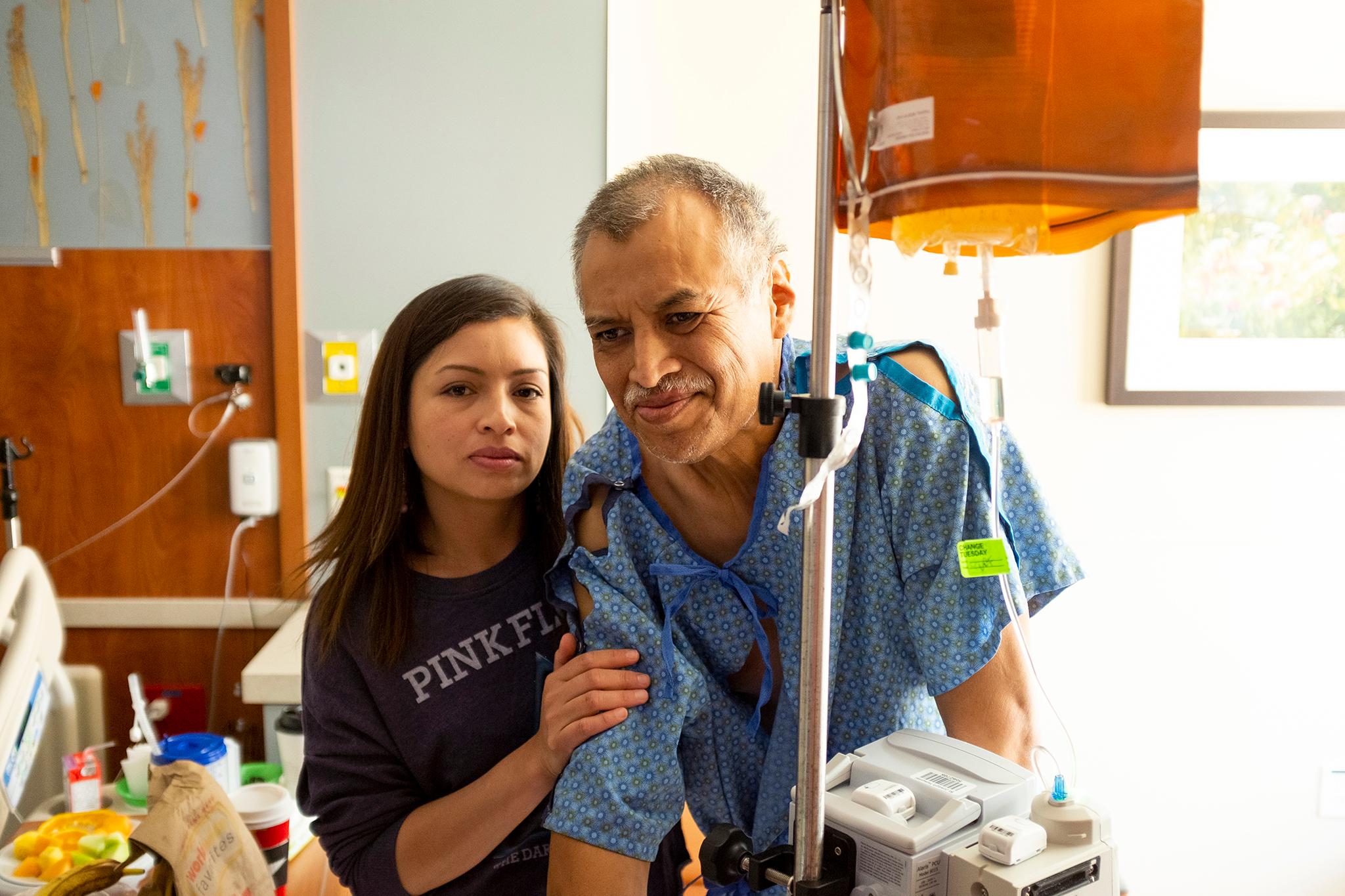
The father's burden was not lifted when they arrived. He worked multiple jobs, at all hours, for decades. The work was hard. Though he always paid his taxes, he was never eligible for health benefits. Going to the doctor was simply not an option.
"We knew that getting any sort of assistance would be a red flag, and we didn't want to do anything that would put us on the radar," Laura said. "Because we were always looking to the dream of getting citizenship, at some point, and we didn't want any of that to interfere."
Once, when Peniche-Cruz's kidneys gave him trouble, a friend from church saw him at home, off the books. It was the same for occasional dental work.
His children eventually secured temporary status under DACA. Laura works in immigration advocacy and, like she dreamed, she works on documentary projects. Armando Jr. is a librarian in Denver. They and their citizen children now have access to preventative care.
Peniche-Cruz was lucky. He never got sick. Until he did.
Early in 2018, he began to notice blood in his stool. It wasn't long before he was racked with pain, sometimes fainting in agony. He began using the toilet so often he moved his bed next to the bathroom.
In July of 2018, Armando Jr. took his father to North Suburban Medical Center's emergency room in Thornton. His pain was so intense that he collapsed in the parking lot. Nurses rushed out with a wheelchair to fetch him. They examined him but determined nothing was seriously wrong. Peniche-Cruz left with a prescription for hemorrhoid medication.
His pain increased over the next year. He visited a clinic for the uninsured a few times, but each trip ended the same way.
"They wouldn't really look into anything that would require a specialist," Laura recalled.
Jeff Bontrager, director of research for the Colorado Health Institute, said this is something that many more people deal with as they face serious conditions. People without insurance and even those who do qualify for Medicaid often have trouble accessing specialist care. His agency estimates Coloradans miss out on 634,000 needed specialty care visits per year.

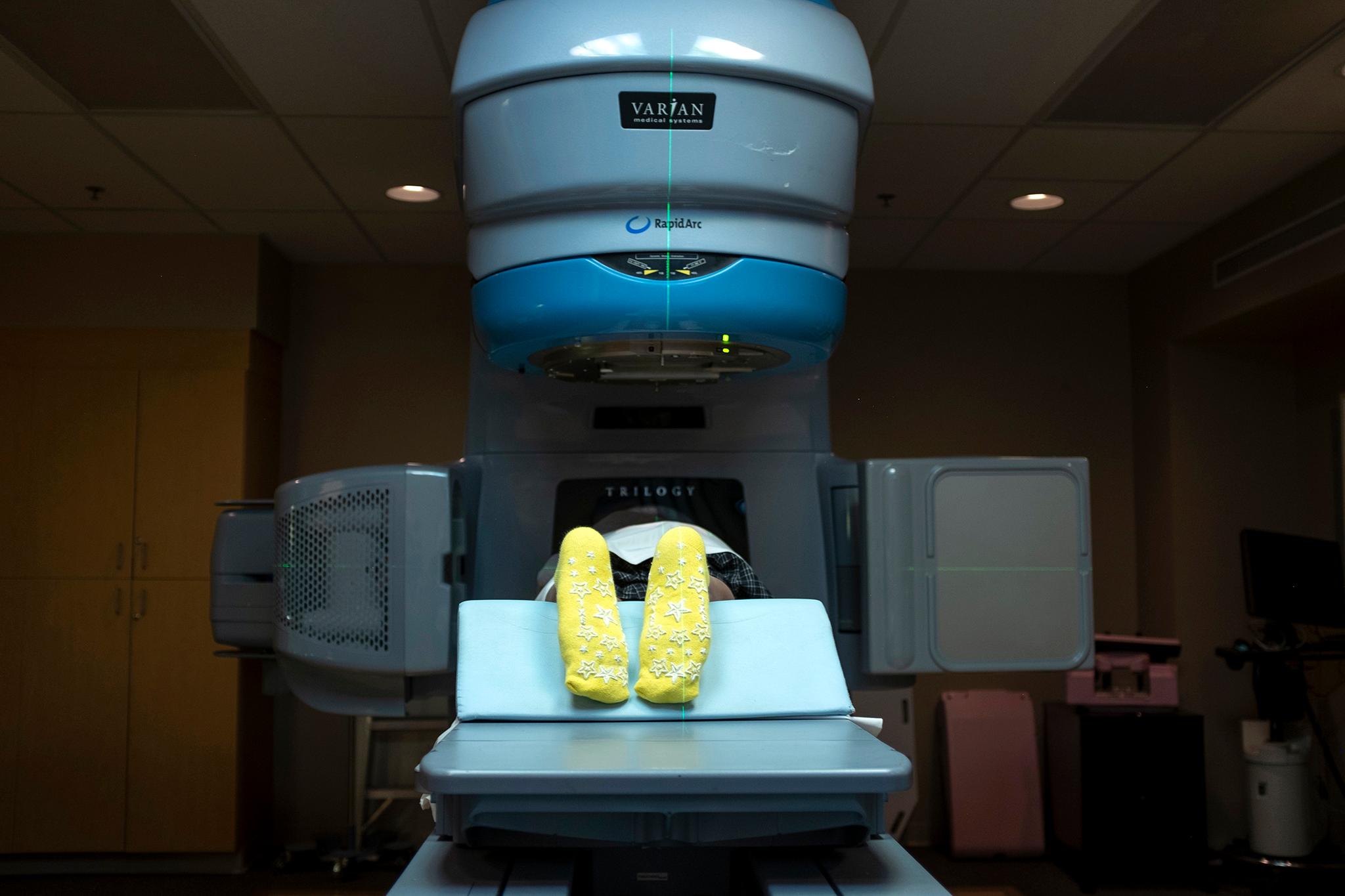
The clinic signed Peniche-Cruz up for a colonoscopy, but the line was three months long. His heath continued to deteriorate as his pain worsened. His kids decided he couldn't wait any longer, so they brought him to another hospital. The staff at Lutheran Medical Center saw him right away. Within minutes, Armando Jr. said, they told him it was definitely not hemorrhoids.
"The doctors were really surprised that the other hospital didn't see the cancer," Laura said. "There's no way that they would have missed that. It's a huge tumor."
They performed emergency surgery, installing the bag on Peniche-Cruz's stomach. But a few more months would drag on before he could really begin treatment.
He bounced around between a few hospitals. Because he was uninsured, Lutheran directed him to Denver Health, the "safety net" hospital serving the city's uninsured. But Denver Health also directed him elsewhere. Even though he has a Denver address, Peniche-Cruz technically resides in Adams County, so they couldn't offer him long-term treatment.
Meanwhile, his worsening pain required attention. Laura took him to St. Joseph's ER. Word was they wouldn't ask about her father's legal status, so she felt safe bringing him there. The clinicians prescribed him some pain killers. He was supposed to begin treatment sometime soon after at Lutheran, which is part of the SCL hospital system with St. Joe's.

The pills ran out before his treatment began. He was hesitant to engage again with the hospital for a refill, so he got some painkillers from a family member. But the medication thinned his blood and caused him to bleed into the bag. He wound up back at St. Joe's emergency room.
There, Peniche-Cruz said, a doctor was shocked that he hadn't begun radiation and made some calls. Doctors told him he'd be allowed to stay at the hospital as he finally received care for his condition. Hospital administrators found charity funds to cover future treatment. After several weeks of radiation, they sent him home. He continues to see doctors for the cancer.
"This is not a story of an individual," said Sarah McAfee, spokesperson for the Center for Health Progress. "This is a story of a broken system that we are all a part of."
Immigration is a divisive issue, today more than ever. But when it comes to healthcare, questions of status turn quickly to questions of economics. Many experts who work within medical systems say everyone would be better off if more people were covered.
Cathy Bradley, an economist who leads the research program at the University of Colorado's cancer center in Aurora, said people without insurance are more likely to be diagnosed with cancer at a late stage. This truism results in two major outcomes.
First, it's more expensive to treat cancer when the disease is more advanced.
"Anytime an uninsured person, regardless of documentation status, comes into our health system, we treat them," she said. "If they come in at a later stage, then we have to treat them more aggressively."
Second, the odds that a patient survives are also "very poor." Emergency Medicaid can cover late-stage treatment, but Bradley said the service is "just above the grave."
The death of a patient is an obvious blow to that person's loved ones, but Bradley said loss also ripples through the local economic system.
"It's a mistake to think of an individual with their particular health need in isolation. Should someone die," she said, "they leave behind children. They are no longer earning. They're no longer paying taxes and we have to care for the people that they supported. It's rarely that we live in isolation, so another person's healthcare needs should be important to all of us."


Sarah McAfee, spokesperson for the Center for Health Progress, told Denverite that someone will end up paying for uninsured patients who show up at emergency rooms: "Hospitals have to get that from their budget somewhere."
If that hospital is a "safety net" like Denver Health, it's often taxpayer dollars that cover those bills.
McAfee's colleague, Aubrey Hill, works on "systems change" for the advocacy group. She said the Affordable Care Act's arrival in Colorado demonstrated how expanding access could cut costs: Colorado's uninsured dropped by half, which resulted in "more than $400 million saved across the state in terms of uncompensated care."
Many of those left still uninsured, she added, are people without legal status who cannot access Medicaid.
In 2017, the Colorado Health Institute estimated about 441,000 people statewide were still uninsured. About a quarter of them, 112,000 people, were thought to be barred from public insurance because they were undocumented.
Armando Jr. said he has no doubt his father's cancer advanced to stage IV as a result of his difficulty reaching a diagnosis.
"If he would have caught it early, the last hospital visit, the first one at North Suburban or even like a simple doctor check-up," he said, "it would have probably prevented a lot of headaches. A lot of this."
Laura said the stress her father experienced in his rollercoaster ride through four area hospitals also took a toll on his health.
"Every time someone said, 'No we can't see you,' that increased his pain," she said. "I could see his pain taking over his body again."

For some, like Laura's father, fighting through the system's obstacles is worth the hassle. But not everyone can cut through the red tape.
Laura's mother, who asked not to be named in this story, ultimately decided to stay in Mexico as her family journeyed north all those years ago. But the distance from her children caused her to change her mind, and she eventually crossed the border to reunite with them. Over time, she developed a migraine problem. Sometimes she lost vision. Once, she woke up and couldn't feel her hands. It scared her.
Laura took her mom to an emergency room in Aurora, but clinicians there told her that the condition wasn't life threatening. It wasn't enough to trigger Emergency Medicaid, and she left the hospital empty handed.
"She was feeling so disappointed," Laura said. "That's when she got even more determined that, being here, she was not going to find the dignity that she needed to live healthy."
Laura and Armando Jr.'s mother decided to return to Mexico in 2017. She'd heard the threat of deportation was rising, and the stress took a toll on her body. She hasn't seen her children since.
"We're so sad that she left, and we miss her so much," Laura said. "But at the same time, out there she's getting good healthcare and she's thriving."
Healthcare is a shifting landscape. Some forces may provide more coverage to Colorado's undocumented. Others may drive them further into the shadows.
Marc Williams, a spokesperson for Colorado's Department of Health Care Policy and Financing, said you'd be "hard pressed" to find any medical professional who thinks uninsured or undocumented residents shouldn't have access to care. But expanding coverage to those uninsured or undocumented will require a political solution.
Colorado's legislature passed a measure last year directing its agencies to explore a state-run insurance plan known as a "public option." The state held 12 public meetings between May and August. The public comment period, which ended Aug. 30, resulted in 30 submissions asking for a range of considerations from ways to keep the system cheap to including dental care.
Four of those comments explicitly requested that undocumented residents be included. Some also asked that Colorado's Division of Insurance remove the "Social Security Number" field from its application to access the private insurance market, saying it would deter people without a number from signing up.
Rep. Dylan Roberts, who co-sponsored the bill, told Denverite undocumented residents would have access to a public option unless it specifically excluded them. But he hasn't seen any proposal drafts yet, and advocates are still writing in to make sure an exclusion doesn't happen.
"I think if you are silent on the issue then it means anybody can purchase the plan if they are able to afford it, regardless," Roberts said. "So I hope that's the way it is. I don't think we need to put guardrails on this as far as immigration status, you know, this is about healthcare, not immigration."
Rep. Marc Catlin, a Republican who co-sponsored the bill, said his interest in a public option is in bringing less expensive insurance to rural areas that can currently only access expensive plans from a single provider. That's Robert's motivation, too. Both legislators said the fact that undocumented immigrants may get access, potentially allowing a quarter of the state's uninsured to attain coverage, hadn't really occurred to them.
Adela Flores-Brennan, executive director of the Colorado Consumer Health Initiative, was one who signed on to a letter representing a number of organizations' requests that undocumented people be included in a potential plan. She said officials should "really think hard about who's most vulnerable" as they near a proposal and include both those who can't afford insurance and those barred from it due to status.
"We believe that if we build a plan specifically designed to benefit people facing the greatest barriers, then the benefits of the new public option will extend to others as well," the letter reads. "As such, we encourage the state to include all Coloradans regardless of immigration status."
Access to something like a cheap public option may have been a help to someone like Peniche-Cruz, who relies on Emergency Medicaid. It would have allowed him access to preventative care. It also would allow him to deal with a state system that's not subject to the whim of federal policy.
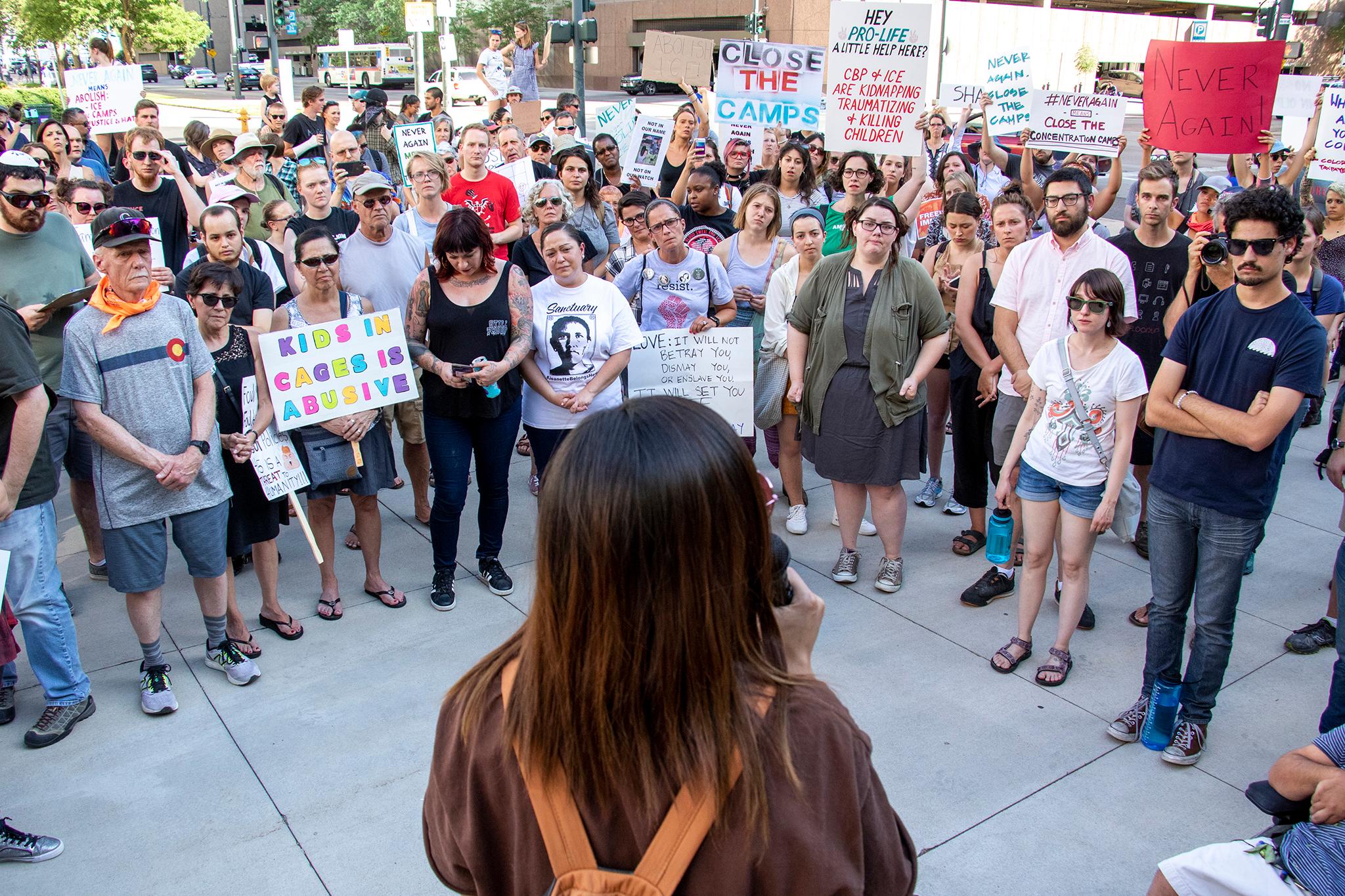

In August, President Trump's administration announced new rules for legal immigration that may bar people who need access to public benefits from citizenship. The policy change was encapsulated in a statement by U.S. Citizenship and Immigration Services' acting director Ken Cuccinelli, who revised Emma Lazarus' famous poem: "Give me your tired and your poor who can stand on their own two feet and who will not become a public charge."
The policy change came to be known simply as "public charge." A person applying for legal residency who might draw on benefits like food stamps or who needs cash assistance could be disqualified from the process. Emergency Medicaid is not on the list, but advocates like Hill, from the Center for Health Progress, said people will still be scared away from that coverage.
"Public charge has had an effect long before the rule was even finalized. It's creating much fear and confusion," she said. "The high levels of fear are on encouraging people to withdraw from society and the supports they need to thrive. It is having that effect now."
Trump's administration began talking about the rule change in 2018.
Vicky Garza is a case manager at Clínica Tepeyac. The community health center located in Globeville serves uninsured patients in the city, some of which are undocumented. Garza said fears of a public charge crackdown last year resulted in patients refusing Emergency Medicaid coverage. Many of them were pregnant women, who would have easily been accepted into the program. Delivering a baby without complication, she said, can cost as much as $12,000.
"People are fearful for accessing those resources," Garza said. "There was a big decline for even accessing something that was available."
There's one other way coverage could be expanded for Colorado's undocumented residents. The services Emergency Medicaid may pay for varies by state. Some, like Washington, cover a broad range of services.
Earlier this year, Denver Health hospitalist Dr. Lilia Cervantes led a successful effort to expand Colorado's program so that uninsured patients in need of kidney dialysis could be treated with the same standards as everyone else. She said further expansion could be possible, but it will probably require additional research to make the case that costs and mortality rates would be eased if other conditions were covered.
"It doesn't take just a healthcare champion or just patient stories. You really have to sort of work collaboratively as a group with health policy stakeholders, Colorado Medicaid, everyone has to partner together," she said.
Despite his struggles, despite his illness, Peniche-Cruz said it's still all worth it.
Armando Peniche-Cruz is back on his feet, though he still looks a little frail. He's still battling the cancer, but the surgery, radiation and weeks spent in a St. Joseph Hospital bed has put him on a pathway to recovery.
A few weeks ago, Armando Jr. and Laura took their father to a park near his home. His granddaughter, Athena, skipped ahead of him on the path as he shuffled to a picnic bench beneath trees chittering with cicadas.
It had been a long year. But his family had surrounded him. He thanked God that they'd managed to push him through the obstacles, to a diagnosis and into treatment.
"It was hard but right now I'm very optimistic," he said. "We did it. We did it because it's not only me."
It was the burden they shouldered in gratitude for the struggles he endured to provide for them. His kids, he said, call his generation the "original Dreamers."
"Because they're dreaming. I want something better for us. I came here not for me. I came here for better opportunity for my kids," he said, "a better life for them."


Athena would start kindergarten in just a week. Peniche-Cruz beamed as she jumped onto the bench next to him.
He asked her: "Are you excited to go to school?"
"Yes!" she replied.
"She's growing so pretty, and so intelligent and so smart," he said to her.
"Thank you," she replied.
He said: "You're welcome."
Correction: Marc Williams' title was originally incorrect in this story. The language describing the Colorado Health Institute's findings was also updated for clarity.