In early March, a mask-free Mayor Michael Hancock gathered with mask-free reporters in his office and said economic trends would inform the city's response to the coronavirus pandemic. As the disease spread, he later ordered businesses to close and residents to stay at home -- decisions that saved lives but gutted the city's economy.
Now, Denver is wading deeper into the third and strongest wave of the coronavirus pandemic, and the tension between the city's physical health and its economic health is again pulling the public in different directions. Close things down, and health professionals say they'll save more lives, but people will lose their paychecks, businesses will go under, and city coffers will dry up even more. Keep things open, and the highly contagious and potentially deadly coronavirus will spread faster.
Denver has taken a different approach, imposing a new soft 10 p.m. curfew, a mask mandate, and public gathering restrictions. Bars and restaurants remain open and exposed, as do businesses in pretty much every other sector, from gyms to construction.
"It's challenging because a lot of our patients have less work and they're out of work and many smaller businesses are struggling to pay the bills," said Pamela Valenza, the chief health officer at Clínica Tepeyac, a community clinic in Globeville that offers free COVID-19 tests. "And so it's understandable," she said about the city still being largely open, adding, "I don't know what the right answer is."

Denver's public health director, Bob McDonald, was one of several leaders to urge the state health department to follow its own guidelines and require counties to clamp down further -- even though McDonald and his boss, Hancock, can do so without the state's blessing. They have not called for a new stay-at-home order despite infection rates that are now worse than the early days of the pandemic.
"We may very well have to do (stay-at-home) again," Hancock told Denverite.
The mayor said he will not necessarily wait for the state to act if he feels stay-at-home orders are necessary, but he would prefer to do things as a region to have "the full impact that it needs to have." New restrictions could come in the next week or sooner, Hancock said, depending on "if we feel like there's a more dramatic shift" in infection rates.
The state and city consider several numbers to decide when to impose or loosen restrictions. The two-week cumulative incidence rate, or how many cases there are per 100,000 residents over two weeks, sits near 1,000 cases; according to the state, anything more than 350 cases pushes a county more into total lockdown territory. As of Saturday, Denver saw six days of declining or stabilizing hospitalization rates -- the state wants that figure to be eight days or more. Denver's two-week positive rate, or the average percentage of tests that come back positive over 14 days, is 11.6 percent, which isn't great, but it's in the state's "safer-at-home" area, a level before stay-at-home.
Anuj Mehta, a pulmonary and critical care physician at National Jewish and Denver Health who led the development of Governor Jared Polis's vaccine allocation plan, said restrictions should be considered on a county-by-county basis. He said imposing stricter rules sooner rather than later would work to eradicate the virus quicker, which would help the economy in the long run.
"So the right health care initiatives may actually be the best for the economy in the long-term. They're obviously exceedingly difficult in the short term," Mehta said.
Jeffery Sankoff, an emergency physician at a hospital in Denver, said the state would benefit from "targeted" shutdowns that restrict going out in counties with really high infection rates. Colorado's data is sophisticated enough to pinpoint the places that need restrictions, he said.

Sankoff has been treating COVID-19 patients back-to-back-to back lately. He's irate. People treat the virus flippantly while hospital beds fill up, he said. And while he understands the need for people to get paychecks, he said people who refuse to wear masks and stay away from others have ruined things for the rest.
"It seems to be rugged individualism to the point of extinction," Sankoff said. "And that's really tragic."
Hancock and McDonald said shutdowns can actually harm people, physically and mentally.
"People have lost their jobs and families and livelihoods have been devastated as a result," Hancock said. "While some companies and businesses have found a way to come back, some have not. And we know that for even those that came back, another stay-at-home order could potentially be the death knell for them."

McDonald also tied physical health to the ability to make money and participate in society. Poverty, homelessness, mental health and substance abuse all come into play with government-ordered closures, he said.
"My view, of course, is public health comes first. This has to be about public health," he said. "Now, having said that, I also recognize that the more public health restrictions you put in place, the more public health problems you might have."
Dr. Valenza at Clínica Tepeyac advises her patients to do whatever makes the most sense for them in a situation that seems to have no good answers, especially for the population she serves, which tends to be lower-income residents who work in so-called "essential" industries like restaurants and construction.
"I think the (COVID-19) fears are real, but then the reality of economic instability is also real," Valenza said. "And being in a place where you can't put food on the table, where you can't buy groceries, where you are concerned about eviction, that's real."
Denver hospitals are already experiencing staffing shortages, Hancock said. Doctors Mehta and Sankoff echoed that sober reality, saying that many of their colleagues have left the industry because of burnout and frustration. Others are sick or must tend to sick family members.
"We have an incredible shortage of staff, and that shortage of staff means that even though there are physical beds available, those beds can't be filled with patients because there's not adequate staff," Sankoff said about the state of the hospital industry.
On the bright side, Hancock and McDonald view this wave as different because of adequate testing supplies, new treatments, and a better understanding of the disease. They'll be watching staffing levels at hospitals closely to shape their decisions about new restrictions, Hancock said.
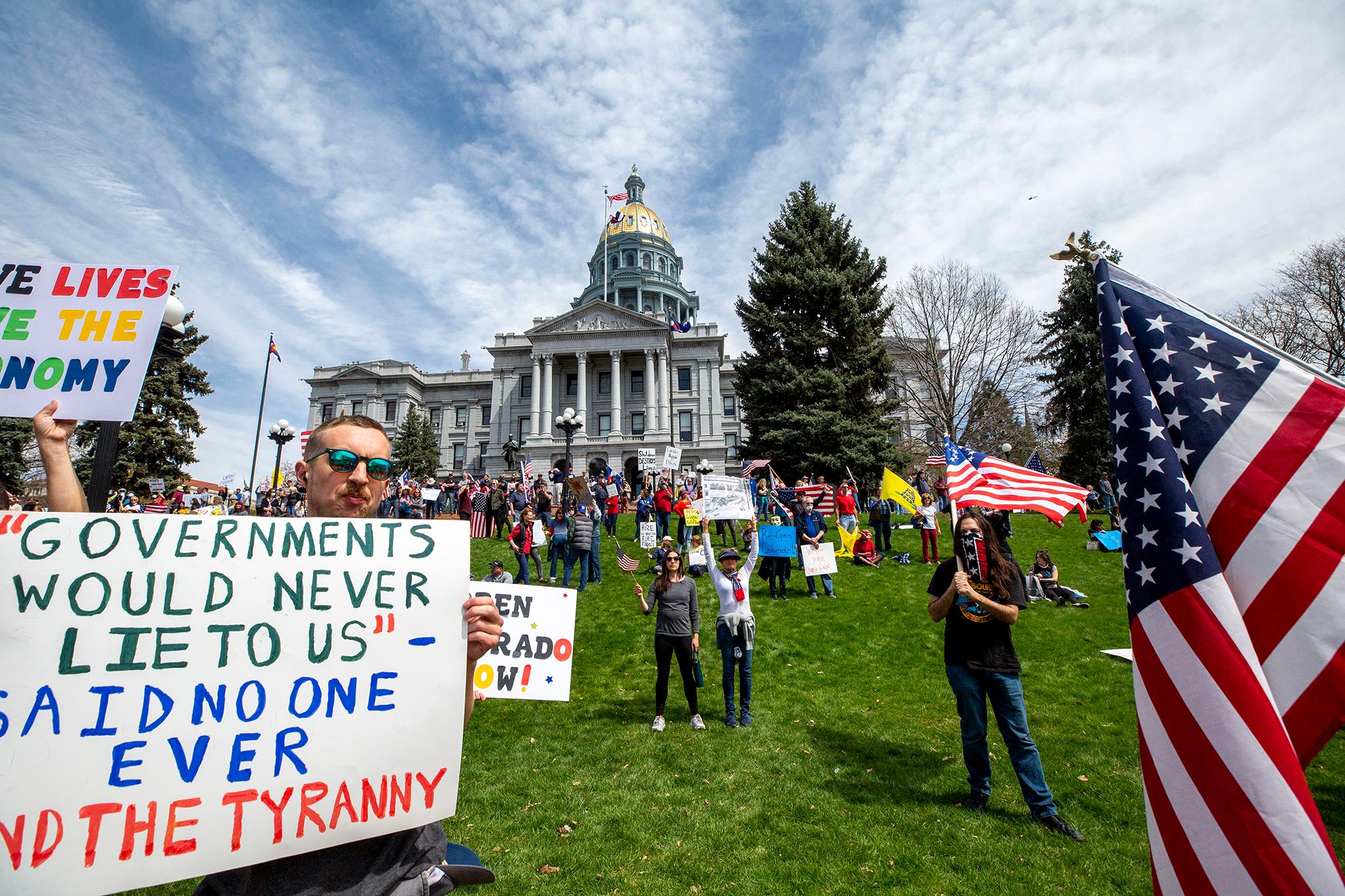
Social safety nets, like another federal stimulus package, could also help the economy. Local, state, and federal governments have provided millions in aid for business owners, renters and others, but it's just that -- aid, not a cure-all.
Everyone from doctors to government officials agree that personal responsibility is key to flattening the curve and staving off heavy-handed restrictions. Wearing masks and staying away from strangers and people outside your household would go a long way toward flattening the curve, according to everyone Denverite spoke to for this article.
But people are still flouting the rules. Healthcare workers say people are spreading the disease indoors at restaurants and bars and at gatherings inside homes.
They also say that misinformation is playing a role. People who believe the disease is a conspiracy theory or being exaggerated by the media and others won't do things like wear masks or social distance, leading to more cases, the physicians said.
"I would challenge anybody that thinks that the pandemic is not real to go to an ICU, sit in a COVID patient's room and hold their hands as they die alone without their family," Mehta said. "And then tell me that it's not real."