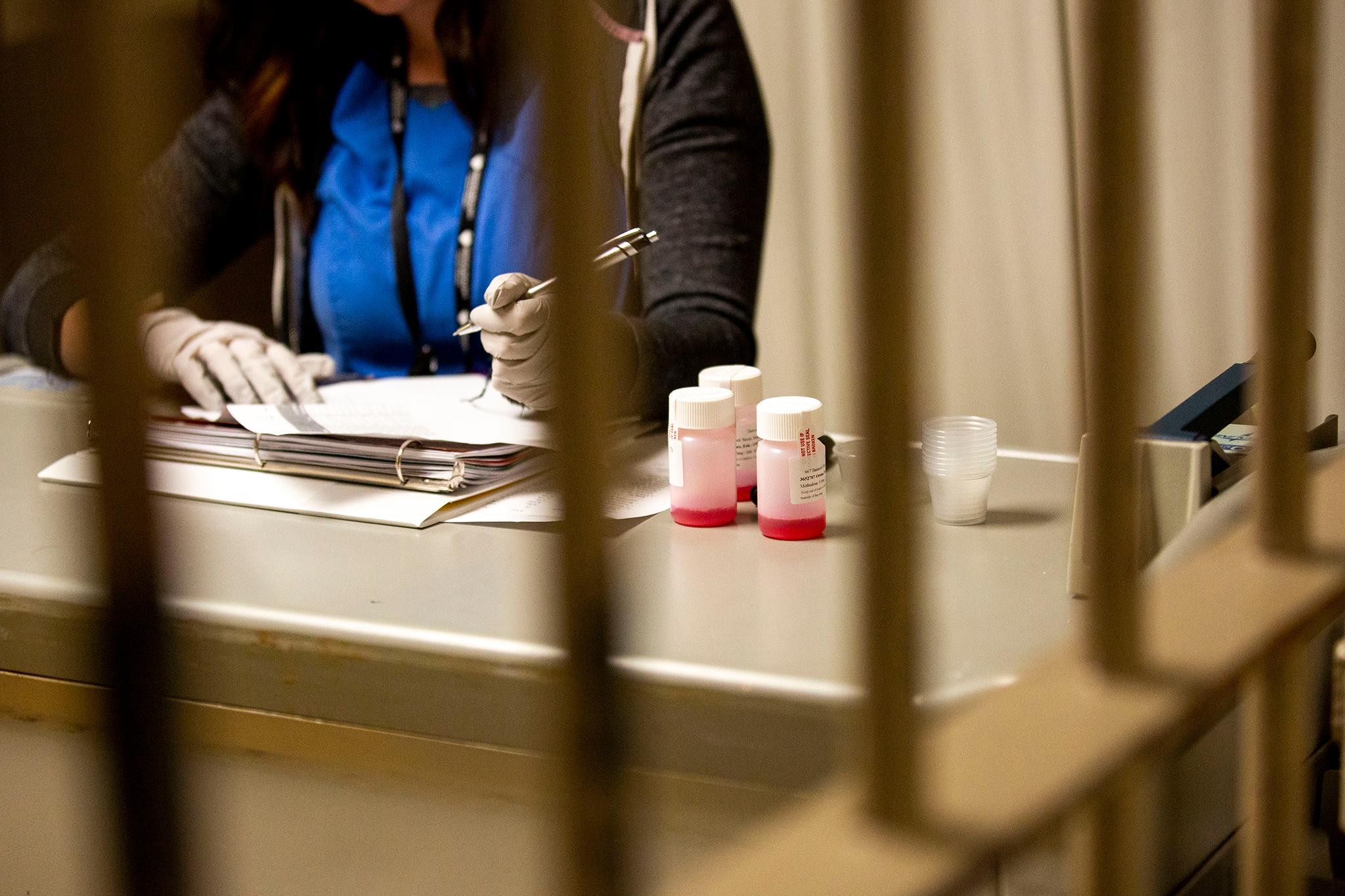
The slow, mechanical hum from the sliding doors leading into Building 4 is a reminder everything inside Denver County Jail is under constant control.
There are no windows here. There is no wall decor. The walls in a hallway leading to the room we're visiting are an ugly shade of orange and something close to yellow. The jail is located in northeast Denver, just north of residential streets in Stapleton.
In here, Denver Health staff help inmates with drug addiction. On a recent Thursday afternoon, inmates walked inside, past those automated humming doors, through another set of doors with metal bars. They stood across from a nurse who asked them their birthday before giving them a dose of methadone, a medication used for people with opioid addiction -- and the program that makes it possible could end up in a lot more places thanks to new funding and what Denver Health says are positive results so far.

No surprise here: If you run a jail, you meet a lot of people with substance abuse disorders.
The Denver Sheriffs Department, which is in charge of local jails, has provided methadone to inmates since at least the early 2000s by partnering with Denver Health. The hospital sends staff to provide medication-assisted treatment -- MAT -- for inmates, which involves using medication like methadone to treat withdrawal symptoms and help someone wean off opioids.
Dr. Sasha Rai, who serves as the Director of Behavioral Health Services for the Denver Sheriff's Department Health Services, said they are looking to expand their treatment program to the Community Corrections facilities -- more commonly known as halfway houses.
Rai said a "significant" number of people who end up at these halfway houses have substance use disorders like drug addiction. Some of the houses already offer treatment options, including MAT.
"Our goal to hopefully include all the facilities from Community Corrections," he said.
Denver Health spokesperson April Valdez Villa said there are two barriers to expanding their program to the halfway homes. First, they will need to make sure there are enough licensed prescribers to staff them and make sure regulatory or licensing needs are met for the halfway homes.
She said she couldn't say how quickly they could make that happen, though the process will involve them and community corrections. She wasn't sure how many halfway homes already have MAT services.
"It is certainly something that we have in our sightlines," Valdez Villa said about expanding.
The program has been growing steadily.
In October 2017, Denver County Jail started offering buprenorphine -- another medication used to treat opioid addiction similar to methadone but not as strong -- thanks to state money.
Rai said this program provided a few days' worth of the medication to help someone with cravings. They were eventually able to expand it in 2018 to provide continued use of the medication, which meant it wasn't tapered off and allowed inmates to get longer treatment.
In September, the Denver Foundation provided a three-year grant to expand its buprenorphine program even more. Denver Health was one of 16 recipients who received $8.4 million in grant money to increase behavioral health care. Rai said the treatment program at the jail is paid for by funding by the state, grants and the jail's own budget.
"We are grateful for the many partners and organizations that share our commitment to broadening access to behavioral health care across the state," Dace West, Vice President of Community Impact at The Denver Foundation, said in a release last year announcing the grant money.
Rai said 1,117 people were put into the opioid withdrawal protocol in 2018, while 322 people were inducted into the buprenorphine program and maintained 319 people on methadone. The department's 2019 annual report showed their average daily population was about 2,110 in 2018.
"We already noticed that we had a large percentage of people coming into the jail that had opioid use disorder," Rai said.
Rai said they found inmates responded better and had a more comfortable withdrawal process with buprenorphine.
"We found patients were much more happier," Rai said. "They didn't have anymore of those withdrawal symptoms like diarrhea, nausea, vomiting."
Rai supervises clinical social workers and staff who work directly with inmates at the jail. The services are offered at both the county jail and the Van Cise-Simonet Detention Center downtown.
Although MAT is essentially the gold standard for treating opioid addiction, it still carries a lot of stigmas.

Rai said inmates saw it as trading one drug for another; yet when more inmates starting using buprenorphine, he noticed they were more likely to use it outside the jail and continue medicating to help with their withdrawals and cravings.
The jail can even continue providing the medication if someone is arrested and end up in jail but was using the medication. Denver Health now has the capacity to continue treatment for inmates who are transferred to other jails.
Denver Sheriff Department Captain Shayne Grannum has been with the department for 25 years and oversees the medical units at both jails. He said it's important to provide these services, which he said can save lives.
"I know our program is one of the first and foremost around the nation with Dr. Rai," Grannum said. "Other agencies are catching up, and that's why there is more coordination between agencies if someone is going from say, Denver to Arapahoe county, or Denver to Jefferson county. Everybody is starting to catch up and we are all on the same page now."
The program doesn't end at the jail. Rai and his staff can provide the medication for people released with a subscription and a referral to Denver Health.
"It's not just treating them when they come in," Grannum said. "It's following them through the whole (treatment) cycle and then transitioning them out in the community."